 Testosterone undecanoate therapy for 30 weeks improves sexual function in men with type 2 diabetes and severe hypogonadism (HG), British researchers concluded. Geoffrey Hackett, MD, of Good Hope Hospital, Sutton Coldfield, West Midlands, UK, and colleagues randomly assigned 199 men with type 2 diabetes and either mild or severe hypogonadism to receive testosterone undecanoate (92 patients) or placebo (107 patients). Of these men, 189 completed the 30-week study. Investigators stratified them, by baseline total testosterone (TT) or free testosterone (FT), into mild HG (TT 9.1–12 nmol/L or FT 0.18–0.25 nmol/L) and severe HG (TT 8 nmol/L or less and FT 0.18 nmol/L or less) groups. They also stratified the men by intervention (placebo or testosterone undecanoate). Dr Hackett's group observed significant improvement in erectile function—as measured using the 15-item International Index of Erectile Function (IIEF)—only in the severe HG group after 30 weeks of treatment with testosterone undecanoate, according to an online report in BJU International. The IIEF score in these patients rose from 9.1 at baseline to 13.0 at 30 weeks. Intercourse satisfaction and sexual desire scores in the severe HG group were improved at 6, 18, and 30 weeks, the investigators reported. Testosterone undecanoate did not change orgasmic function in any of the patient groups. The authors concluded that their study endorses the view of the Endocrine Society that the burden of hypogonadism-related sexual dysfunction in men is evident at TT levels of 8 nmol/L or less. The present findings also suggest that therapeutic trials of testosterone replacement therapy, especially with testosterone undecanoate, should be more than 30 weeks' duration, not 3 months as suggested by some guidelines, the researchers wrote.
0 Comments
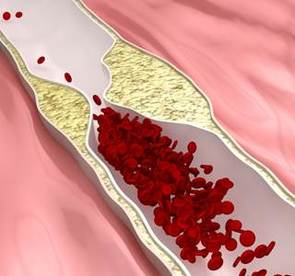 Men with low or low-normal testosterone levels who received testosterone replacement therapy for 3 years as part of a study experienced no significant change in subclinical atherosclerosis progression. They also had no significant improvement in overall sexual function or health-related quality of life (QOL). Researchers led by Shalender Bhasin, MBBS, of Harvard Medical School in Boston, randomized 156 men to receive 7.5 g of 1% testosterone gel and 152 to receive placebo gel packets daily for 3 years. Patients had a mean age of 67.6 years. To be included in the study, men had to have testosterone levels of 100–400 ng/dL or free testosterone levels less than 50 pg/mL. The co-primary outcomes were the rate of change in distal right common carotid intima-media thickness and coronary artery calcium. The rate of change in carotid artery intima-media thickness was 0.010 mm per year in the placebo group and 0.012 mm per year in the testosterone group, Dr. Bhasin's group reported in the Journal of the American Medical Association (2015314:570-581). The rate of change in the coronary artery calcium score was 41.4 Agatston units per year in the placebo group and 31.4 Agatston units per year in the testosterone group. None of these between-group differences were statistically significant. The researchers assessed sexual function using the International Index of Erectile Function, a validated 15-item questionnaire that assesses 5 domains of sexual function (erectile function, orgasmic function, sexual desire, intercourse satisfaction, and overall sexual satisfaction). They used the Medical Outcomes Study 36-item short form health survey (SF-36) to assess health-related QOL. Dr. Bhasin and his colleagues found that testosterone administration did not significantly improve erectile or ejaculatory function, sexual desire, partner intimacy, health-related QOL. Intercourse satisfaction showed statistically significant improvements, but these “were of small magnitude and could be due to chance alone, in light of the lack of improvements in other domains of sexual function.” “Because this trial was only powered to evaluated atherosclerosis progression and not cardiovascular events, these findings should not be interpreted as establishing cardiovascular safety of testosterone use in older men such as those enrolled in this trial,” the authors cautioned. |
Σχετικά
Με το ιστολόγιο αυτό επιχειρείται η κατά το δυνατόν άμεση ενημέρωση σε θέματα που αφορούν ουρολογικές εξελίξεις και δίνεται η δυνατότητα σχολιασμού των αναρτήσεων. Κατηγορίες
All
|
|
Ιατρείο Λαγκαδά: Δ. Μήλιου 24 (έναντι 1ου δημοτικού), Λαγκαδάς
Τ: 2394 020 780, Κ: 693 63 23 794 |
Όροι Χρήσης | Επικοινωνία | Copyright © 2013
 RSS Feed
RSS Feed