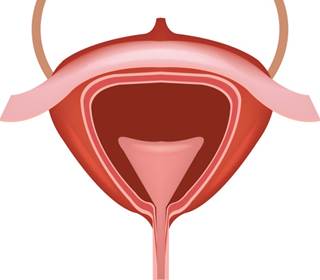
 Research conducted by scientists at the University of York has revealed how recreational ketamine abuse damages the bladder. In two studies, one of which is published today, the team shows how ketamine present in urine causes damage to the epithelial lining of the bladder, allowing urine to penetrate into underlying tissues which causes inflammation and extreme pain. In some cases this pain can be so extreme that patients need to have their bladder removed (cystectomy). Led by Dr Simon Baker in the University of York's Department of Biology, in collaboration with clinicians from Middlesbrough and Leeds hospitals, the first study looked at a cystectomy case. This would determine whether bladder damage was caused by direct contact with urinary ketamine or whether the drug causes a systemic change in the whole body that affects the organ. Reporting a rare physiological coincidence, the team studied epithelial cells lining the bladder and also in an adjacent remnant of the foetal urinary tract, not in contact with urine, known as an urachus. Finding that epithelial cells lining the bladder were almost completely absent, having died and been sloughed off into the urine, epithelial cells from the urachus appeared healthy. This shows direct contact with urine is critical to the toxicity of ketamine to the bladder epithelium, ruling out systemic factors. In the second study, the researchers used epithelium cells taken from healthy patients to study how ketamine affects the bladder. Used to produce laboratory models, cells were exposed to ketamine and their responses analysed. The researchers found that ketamine overwhelms the cell's internal power stations, known as mitochondria, causing a catastrophic release of toxins. To avoid this "melt-down", cells commit a controlled form of suicide (apoptosis) resulting in cell death. This occurs in a regulated fashion that does not cause excessive toxicity to other cells in an attempt to protect the remaining tissue; however, in the case of chronic ketamine abuse, all epithelial cells are killed. Dr Baker, Senior Postdoctoral Research Fellow in York's Jack Birch Unit for Molecular Carcinogenesis, said: "These two studies combine to demonstrate that direct contact with urinary ketamine causes significant bladder damage, and shows how this drug causes the death of previously healthy bladder cells. "We now have a more detailed understanding of how and why chronic ketamine abuse results in bladder problems and cystitis. Understanding the full side-effects of ketamine is very important as other researchers are currently investigating the potential for this drug to spawn a new generation of anti-depressants." Ketamine poisoning of the epithelial lining can lead to extreme pain associated with ketamine cystitis. Urologists advise anyone who experiences bladder pain when using ketamine to stop taking the drug immediately, as if too many bladder cells are killed there will not be enough remaining to repair the tissue.
0 Comments
 The unraveling of the human genome has triggered a shift toward classifying cancer according to patterns found in molecules and genes rather than cells and tissues. An example of this is a new study that defines a new subtype of bladder cancer that shares molecular signatures with some forms of breast cancer. Researchers from the University of North Carolina (UNC) at Chapel Hill describe how they arrived at the new definition in the journal JCI Insight. Bladder cancer accounts for about 5% of all new cancers in the US. It is the fourth most common cancer in men, but it is less common in women. Estimates suggest that during 2016, about 76,960 Americans will discover they have bladder cancer, and about 16,390 will die of the disease. The wall of the bladder has four layers. Nearly all bladder cancers start in the urothelium - the innermost layer. Next to the urothelium is a thin layer of connective tissue, blood vessels and nerves, followed by a thick layer of muscle. The outside layer - made of fatty connective tissue - separates the bladder from other nearby organs. As the cancer grows, it spreads from the innermost layer into and through the other layers. The more layers it penetrates, the more advanced the cancer is and the harder it is to treat. Patients diagnosed with muscle-invasive and metastatic tumors have a much poorer prognosis than patients with low-grade tumors that are largely confined to the inner layers of the bladder wall. Signatures of immune suppressionIn the study, senior authors William Kim and Benjamin Vincent, of the Lineberger Comprehensive Cancer Center at UNC, and colleagues found that a subtype of muscle-invasive bladder cancer shares molecular signatures with some forms of breast cancer. It was already known that a subset of triple-negative breast cancers expresses low levels of a protein called claudin. In the new study, the researchers show that claudin-low tumors also represent a specific subtype of bladder cancer. The team arrived at the finding with the help of data from The Cancer Genome Atlas (TCGA). They used the gene signatures that define claudin-low tumors in breast cancer to search TCGA data-sets obtained from 408 high-grade, muscle-invasive urothelial bladder carcinomas. They also found that the claudin-low tumors were rich in a group of gene signatures that showed the immune system had managed to penetrate the tumors. However, despite this high immune presence, it appears the cancer cells had suppressed the immune cells by blocking their "checkpoint" molecules. Immune checkpoint molecules are an important feature of the immune system. To ensure they attack the correct targets and not healthy cells, immune cells that do the attacking sport these "switches" on their cell surfaces. The checkpoints are activated (or inactivated) by patrolling immune cells. However, some cancer cells find ways to use these checkpoints to avoid being attacked by the immune system. There are drugs available - called checkpoint inhibitors - that target the checkpoints to "de-repress" the immune system, and they hold a lot of promise as cancer treatments. The authors conclude: "These finding suggest that claudin-low bladder cancers may be particularly responsive to immunotherapy-based treatments that de-repress the immune system. Future studies will be needed to clinically test immune checkpoint inhibitors in this population." Meanwhile, Medical News Today recently learned how experts from around the world are making progress on agreeing a way to classify bladder cancer according to genetic and molecular - rather than cell and tissue - features. |
Σχετικά
Με το ιστολόγιο αυτό επιχειρείται η κατά το δυνατόν άμεση ενημέρωση σε θέματα που αφορούν ουρολογικές εξελίξεις και δίνεται η δυνατότητα σχολιασμού των αναρτήσεων. Κατηγορίες
All
|
|
Ιατρείο Λαγκαδά: Δ. Μήλιου 24 (έναντι 1ου δημοτικού), Λαγκαδάς
Τ: 2394 020 780, Κ: 693 63 23 794 |
Όροι Χρήσης | Επικοινωνία | Copyright © 2013
 RSS Feed
RSS Feed